Insulin Pumps & Continuous Glucose Monitors (CGM)
Insulin Pump Therapy
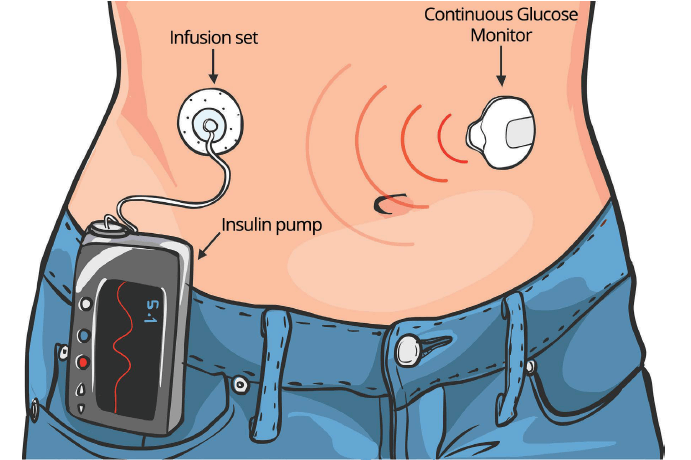
An insulin pump is a small device that delivers insulin continuously (basal) or quickly (bolus) in response to carbohydrate intake. You can also correct a high blood glucose level by entering the amount of blood glucose or grams of carbohydrate to be eaten into the insulin pump. There's a variety of insulin pumps on the market, offering options to meet individual needs.
A pump can help improve blood glucose control, but it is essential to continue checking glucose levels regularly using a continuous glucose monitor (CGM) or a glucose meter.
While the insulin pump continuously delivers insulin, it’s not a cure for diabetes. The goal is to manage your blood glucose levels more effectively while avoiding wide fluctuations and preventing severe hypoglycemia (low blood glucose).
How insulin pumps work
The information in the insulin pump is programmed to meet the individual's specific needs. Insulin is infused into fatty tissue through a small plastic tube, called a cannula, that's attached to a reservoir in the pump. The cannula is inserted under the skin by a needle, which is referred to as an infusion set. It's changed every two to three days to prevent infection. Only rapid-acting insulin is used in a pump. Since the pump continuously delivers insulin, there is no need for long-acting insulin.
Benefits of using an insulin pump
Studies indicate that an insulin pump can improve diabetes control and reduce the risk of hypoglycemia. Many individuals find they have greater flexibility with meals and exercise timing when using an insulin pump.
Sharing insulin pump data reports with your care team before office visits allows them to review them with you, identify patterns, and make necessary adjustments to your care plan.
Is an insulin pump right for you?
Candidates for insulin pump therapy typically receive multiple daily insulin injections, check their blood glucose levels several times a day, are motivated to use the pump, and possess good problem-solving skills. Open communication between the person wearing a pump and their diabetes care team is essential.
Insulin Pumps Comparison Sheet
Guidelines for Insulin Pump Problem-Solving
Troubleshooting High Blood Glucose
Insulin Pump Hospitalization Guidelines
Continuous Glucose Monitors (CGM)
Checking blood glucose with a meter only provides information about the blood sugar level at that specific moment. It does not identify patterns or indicate whether blood glucose is rising or falling.
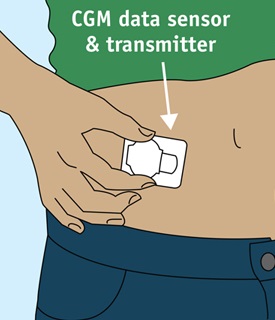
A CGM sensor is inserted under the skin into fatty tissue. It's connected to a transmitter that sends information to a smartphone or receiver. You can view glucose level history, the current level, and the direction it's heading. Trends in blood sugar levels can help you anticipate and prevent high & low blood sugar.
Some CGM sensors even alert the user (and/or family members) when glucose levels become too high or too low.