Obesity Projects with Dr. Jason Kim at UMass Chan Medical School
Role of Cytokines in Energy Balance and Diet-Induced Obesity
Our body weights are maintained by a delicate balance between food intake/feeding behavior and energy expenditure/physical activity. We have developed a chronic high-fat feeding in mice to model type 2 diabetes in humans with respect to diet-induced obesity causing insulin resistance (Park, S.-Y. et al., Diabetes 2005;54:3530-3540). Mice homozygous for the severe combined immunodeficiency (scid) mutation have disrupted the immune system lacking functional T and B lymphocytes. Interestingly, we have recently found that mice with scid mutation are partially protected from diet-induced obesity, and these SCID mice showed increased energy expenditure and physical activity, measured by using metabolic cages after high-fat feeding (Friedline, R.H. et al., FASEB J. 2016;30:1328-1338). We have also found that SCID mice bearing a null mutation in the IL-2 common g chain receptor (NSG), which lack mature lymphocytes and NK cells, are entirely protected from diet-induced obesity and insulin resistance after high-fat feeding. We are currently investigating the intracellular signaling pathways of cytokines and organ-to-organ crosstalk between cytokines and multiple physiological systems to understand the cytokine regulation of energy balance and obesity.


Role of Altered Gut Microbiome in Energy Balance and Obesity
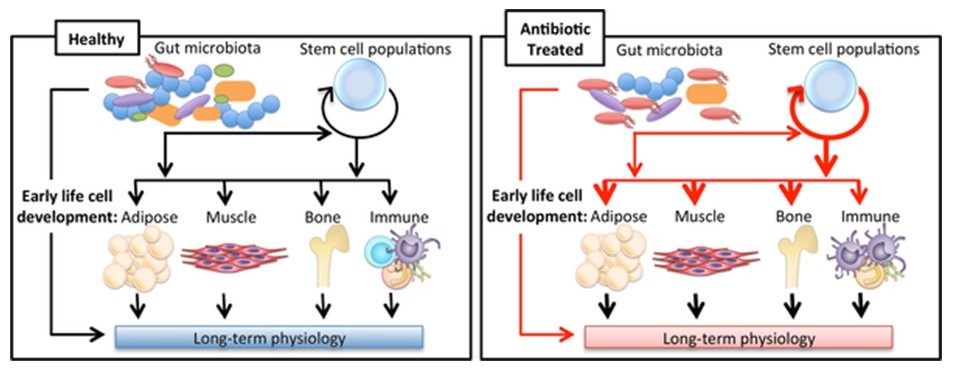
The gut microbiota and their secreted metabolites have profound effects on host energy balance and metabolism. Although recent studies have shown altered gut microbial communities in obese and diabetic humans and animals, their role in the pathogenesis of metabolic diseases remains unclear. We have recently found that antibiotic-mediated alteration in gut microbiota affects energy balance and obesity during chronic high-fat feeding, and these effects are differentially regulated in male and female mice. We have also found that chronic high-fat feeding alters selective gut microbial communities in mice. Using antibiotics, fecal microbiota transplant, and ovariectomy, we are investigating the underlying mechanism of gender-selective effects of altered gut microbiota on energy homeostasis and metabolism.
Role of Leptin Resistance and Signaling in Obesity and Type 2 Diabetes
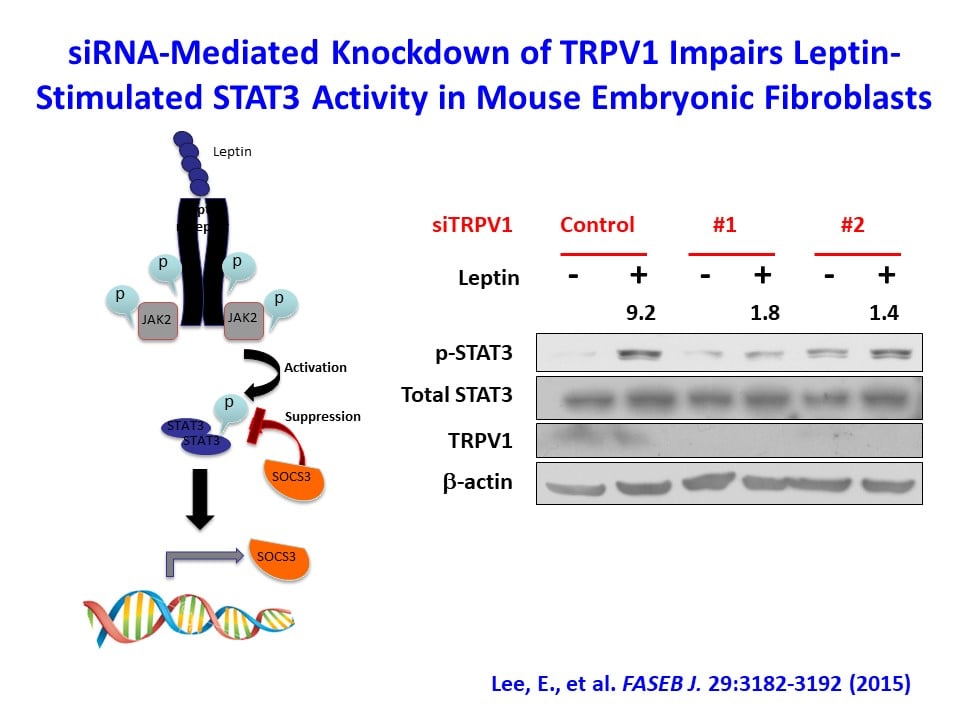
Leptin is an adipocyte-derived hormone (adipokine) regulating our feeding behavior as an appetite suppressant, and leptin resistance is an important characteristic of human obesity. Recent reports have indicated that capsaicin, a major component of chili pepper, may have an anti-obesity effect. The transient receptor potential vanilloid type-1 (TRPV1) channel is a member of the TRP protein superfamily, and capsaicin is a natural and specific agonist for the TRPV1 channel, inducing pain and thermogenic responses commonly known as the spicy sensation. Interestingly, we have recently found that mice lacking TRPV1 channel (TRPV1 KO) develop increased obesity in response to chronic high-fat feeding and become more insulin resistant than wild-type cohorts (Lee, E. et al., FASEB J. 2015;29:3182-3192). The underlying mechanism involves leptin resistance as leptin treatment failed to suppress food intake and hypothalamic STAT3 activation in TRPV1 KO mice. We are currently investigating the molecular basis by which capsaicin and TRPV1 modulate the feeding behavior and their potential beneficial effects against obesity.

Affiliated Centers
Diabetes Center of Excellence at UMass Chan Medical School
Metabolic Disease Research Center