Learning Communities mentors make a personal connection with students

If a job description for the new Learning Communities mentors appeared in a help wanted ad, it might read:
WANTED: Twenty dedicated faculty with clinical experience to guide students through the challenging world of medical school, to offer encouragement, answer career questions and monitor academic progress. Must be able to teach doctoring skills, such as how to conduct a medical interview and physical exam, and solve complex clinical problems. Knowledge of the many support resources available at the Medical School essential, but will train. Reward is the chance to teach, guide and inspire the next generation of physicians.
When Learning Communities co-directors Mike Ennis, MD, and David Hatem, MD, visited academic departments last spring with their own version of this job description, they weren’t sure they could convince enough qualified faculty to try this new way of teaching and guiding medical students. The Learning Communities are an essential element in the School of Medicine’s redesigned curriculum that was launched this fall, but they were concerned that the uncertainty of this new, untested role—plus the significant time commitment—might be a deterrent.
They worried needlessly. Forty experienced faculty members applied for the 20 available positions, and the challenge became choosing from an over-abundance of well-qualified applicants. As hoped, the selection committee was able to create a mentor group that represents the breadth and diversity of the Medical School’s teaching faculty—in terms of experience, gender and departments and professional concentrations represented.
The motives of the mentor applicants were varied, but there was a common theme. “People who go into medicine have a desire to give back. They are interested in knowing, how can we support the development of the next generation of physicians?” said Dr. Hatem, clinical associate professor of medicine. Some remembered their own mentor—usually found through their own initiative or by happenstance—who made a significant difference in their medical school careers. “Others maybe didn’t have a mentor and they would like to provide UMass Medical School students with an educational experience that is potentially less isolating.”
The overall purpose of the Learning Community mentors was also intriguing to the applicants. “They are going to shepherd these students through medical school, from matriculation to graduation. In that sense they are almost more like coaches,” said Dr. Ennis, associate professor of family medicine & community health.
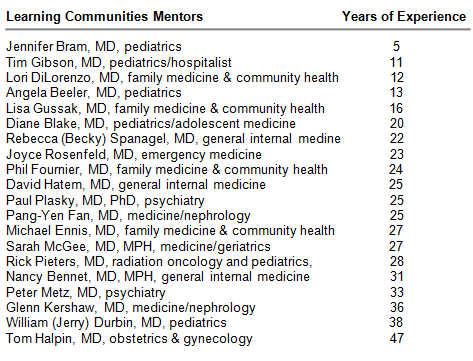 Collectively, the group represents 488 years of experience, with individual experience ranging from five years (alumna Jennifer Bram, MD, assistant professor of pediatrics) to 47 years (Tom Halpin, MD, professor of obstetrics & gynecology), with 75 percent graduating from medical school more than 20 years ago. The nine women and 11 men are members of seven academic departments and represent 11 concentrations. “Most importantly, each has been recognized for outstanding patient care and role modeling as a physician and an educator,” said Ennis.
Collectively, the group represents 488 years of experience, with individual experience ranging from five years (alumna Jennifer Bram, MD, assistant professor of pediatrics) to 47 years (Tom Halpin, MD, professor of obstetrics & gynecology), with 75 percent graduating from medical school more than 20 years ago. The nine women and 11 men are members of seven academic departments and represent 11 concentrations. “Most importantly, each has been recognized for outstanding patient care and role modeling as a physician and an educator,” said Ennis.
Eventually, each mentor will be responsible for six or seven students from each of the four class years, for a total of 25 students. Only the first- and second-year classes are paired with mentors in the Learning Communities so far, so each mentor is focused on 12 or 13 students for now. They meet with their students on a regular basis to discuss career goals, the stress of medical school, where to get academic help—even how to get around the city of Worcester.
“This is really allowing us to see the student as a person rather than just someone trying to master skills,” said Hatem, who, along with Ennis, is also a mentor. “Both faculty and students are better connected.”

Four months in and the experience has been as rewarding as advertised. “It’s been a lot of fun. I’ve connected best with the first-year students because they need a little more help since they are adjusting to medical school,” said Pang-Yen Fan, MD, clinical associate professor of medicine, who also brings to the table his experience as director of the nephrology fellowship. “When we get closer to the end of the academic year and we start talking about transitioning to clinical rotations, we will be a lot more help to the second-year students.”
For Dr. Bram, the opportunity to teach the first-year students is what excites her most about being a mentor. Although the youngest of the group, her previous experience as chief resident uncovered a love of teaching that makes the personal connections even richer. Besides advising and career counseling, the mentors teach longitudinal classes, such as Doctoring and Clinical Skills, the former Physician, Patient and Society class that teaches foundational patient care skills.

“I have a different perspective on what it means to be a medical student. I’ve been there most recently and I can relate,” she said. The fact that she is an alumna is also important. “I know the system and the people.”
In the past, the advising system relied on hundreds of volunteer advisors, many of whom were not closely connected to their advisees. Now mentors are clamoring for information about how their students are performing academicially even before test scores are returned, said Ennis. The fact that mentors are paid—eventually up to 25 percent of their time may be funded through the Learning Communities budget—gives all three functions (mentoring, teaching and being part of the student community) the proper value, he said, adding that students will likely have much less difficulty deciding whom to ask for a recommendation for their residency applications.
Officially, the Learning Communities are broken into five houses—Burncoat, Tatnuck, Kelley, Quinsigamond and Blackstone. An unplanned development is the creation of another unofficial community: the mentors themselves. Each Wedneday, they meet as a group to learn about the skills and resources that will help their students get the most out of their experience.
“We all have a different way to approach things. It is helpful to hear other ways of handling problems or issues, and that’s been very positive,” said Dr. Fan. “You don’t have to know everything, you just have to know where to get the help.”
The most moving experience for the mentors so far might have been their first official duty: putting the white coats on their first-year mentees during the Medical School’s first White Coat Ceremony in September. Each student crossed the stage to meet his or her mentor, who welcomed the student into the UMMS academic community.
“I felt really honored to be there and be the person to mark the beginning of their medical school journey,” said Bram. “It was a powerful symbol to have the mentors be a part of that ceremony.”